Jessy is a 28-year-old diabetic who was bitten by her cat at the base of her thumb. She presents to the emergency department 12 hours later with a swollen, tender, and erythematous right hand and explains that she came in because she thinks she has blood poisoning. She is afebrile and normotensive with a pulse of 68 beats per minute, a blood glucose level of 18 mmol/L, and a nontoxic appearance.
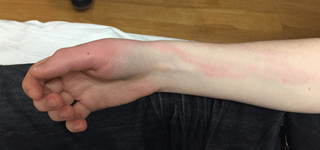
Figure 1: Jessy’s erythematous and swollen right hand
On examination, she has four small puncture wounds along the dorsal aspect of the base of her right thumb with erythema and tenderness in her index finger and lymphangitis along her arm.
More than half of all Canadian households include a pet, with a slightly higher prevalence of cats than dogs.1 Animals provide excellent companionship for humans, and there are measurable health benefits to pet ownership.2–4 However, there are also risks associated with living or interacting with animals, including infections, abrasions, and falls; more than 75% of reported injuries result from bites.5 Risk factors for dog bites include young age, male sex, dog ownership, and contact with certain breeds, unneutered male dogs, dogs involved with protection of food or property, and leashed dogs.6 The most common bite location is the face.7
Animal bites account for a significant number of visits to emergency departments worldwide. Dog bites alone account for 1% of reported injuries in Canada, approximately 30,000 visits per year; they have a hospital admission rate of 2.5% and carry a death rate of 0.007/100,000.8–11 The need for health care professionals to have up-to-date knowledge and skill in caring for these injured patients is evident.
Patients with severe injuries requiring resuscitation or airway management should have the bite wound assessment deferred to the secondary trauma assessment. Animal bites must be carefully assessed. Some patients require greater caution in both management and follow-up. Patients with a decreased immune response, which can result from diabetes, asplenia, immunosuppressant therapy, and peripheral vascular compromise, are at an increased risk of infection.
All patients should have vital signs taken and have their tetanus immunization status documented and updated, if indicated. For previously immunized patients, a booster dose of tetanus toxoid is recommended for minor, clean wounds if ten or more years have elapsed since the patient’s last vaccine. For all other wounds, a booster should be given if five or more years have elapsed. In addition, patients who have had an unknown number, or fewer than three, doses of tetanus toxoid must also receive tetanus immune globulin to provide immediate passive protection.11
A thorough evaluation for injury to functional structures is an essential part of any bite wound assessment; this must include inspection of the wound for foreign bodies, evaluation of neurological and vascular status, and exploration for tendon and joint involvement. If there is any suspicion of a retained foreign body, an x-ray should be performed. Prophylactic antimicrobials are indicated for patients with a high risk of infection and wounds that are infected at the time of initial presentation or sutured.13
All bite wounds should be cleaned with a povidone-iodine solution to reduce the bacterial and viral load in the wound. Cleaning bite wounds should include irrigation with 100 to 200 ml of tap water using a 19-gauge needle and syringe to achieve a pressure of 7 lb/in2.12
Suturing may be undertaken on the face or other areas where cosmetic outcome is of high importance. It is inadvisable to suture bites that are more than eight hours old and wounds associated with crush injury, puncture-type wounds, hand bites, and cat or human bites. Victims at high risk for infection should also not receive sutures.
Follow-up instructions are essential in all bite wounds. Patients should be advised to return if they have increasing pain or loss of function or if the wound drains purulent material or is erythematous.
Dog are responsible for 85 to 90% of recorded animal bites.13 They cause a greater number of admissions and account for more bite deaths than all other bites together. In contrast to cats, dogs typically bite with greater force, and there is often an associated crush injury. Pit bull terriers, Rottweilers, and German shepherds account for the majority of dog bites, and offending dogs are typically familiar with the victim before the bite occurs.13 Essential history includes the nature of the interaction with the animal, the dog’s vaccination status, and the patient’s vaccination status.
Knowing whether to suture dog bites in cosmetically important areas, such as the face, arms, or hands, is critical. Recent evidence supports primary wound closure after cleansing within eight hours of the injury.14
Prophylactic antimicrobial therapy is rarely indicated and should be reserved for high-risk injuries to the hands and face and for immunocompromised or asplenic patients. Follow-up is important as dog bite infections typically occur 24 hours post injury. Infected dog bites are polymicrobial from canine oral flora and often contain species of Pasteurella (50%), Streptococcus (46%), and Staphylococcus (46%).15 One rare pathogen, Capnocytophaga canimorsus, is of particular concern as it can cause septicemia in immunocompromised patients. Out-patient oral monotherapy with amoxicillin and clavulanic acid is usually effective for these infections and remains the therapy of choice for all patients with dog bite injuries, when indicated. In penicillin-allergic patients, doxycycline alone or a combination of clindamycin and fluoroquinolone are effective alternatives. For inpatient therapy, piperacillin/tazobactam or clindamycin/ciprofloxacin is indicated.
Cats’ long sharp teeth allow deep penetration of bacteria without aeration. This is of particular concern in cat bites to the hand and for injury to superficially located essential structures (vascular structures, tendons).13 Infections resulting from cat bites usually develop more rapidly than infections in other animal bite injuries, typically within twelve hours; wound closure is, therefore, not advisable.13 As with dog bites, cat bites are also polymicrobial and associated with Pasteurella (75%), Streptococcus (46%), and Staphylococcus (35%).15 Outpatient monotherapy with amoxicillin and clavulanic acid is usually effective for these infections and remains the therapy of choice. In penicillin-allergic patients, doxycycline is effective. For inpatient therapy, ceftriaxone is indicated. In immunocompromised patients, cat bites require next-day follow-up and clear advice to return earlier if symptoms and signs of infection develop.
Bites from squirrels, gerbils, guinea pigs, and rabbits should be treated like cat bites.16
Although dogs may carry the rabies virus, rabies is rare in domestic animals. Bat rabies transmission is more likely via coyote, raccoon, skunk, or fox bite.13 Washing the bite wound with a povidone-iodine solution effectively reduces the viral load and is recommended if there is concern about rabies. A 10% solution (diluted 10:1 to 20:1 with tap water) is ideal for cleansing and irrigating these wounds.
Since 1989, physicians have struggled to adhere to the “bat in the room while sleeping” indication for rabies prophylaxis. The number needed to treat for this therapy is 314,000 exposures (and is likely closer to 1.9 million as conservative estimates were used), making it an unwise choice for patients.17 Rabies vaccination is still indicated for patients without prior rabies vaccination who have been bitten by a bat.
Local public health authorities should be contacted immediately to provide direction for case management.18 Four doses of the rabies post-exposure vaccine should be administered over the first few weeks after the bite; one additional dose is necessary in immunocompromised patients.19
Patients with animal bites may require admission for severe infections, systemic symptoms, failure of outpatient therapy, immunocompromised state, infections involving tendons, bones, or joints, and noncompliance with therapy.

• Animal bites are common injuries for which effective and directed history, clinical assessment, management, and follow-up are important
• Consideration of patient and animal factors in managing these wounds leads to safer care
•Prophylactic antimicrobials are generally unwarranted unless there is an increased risk of infection (e.g., cat bites or immunocompromised victims)
• Some dog bite wounds may be judiciously sutured to achieve an acceptable cosmetic outcome
• Rabies vaccination is no longer recommended for patients who have been in a room with a bat and should be reserved for patients with bat bite injuries
1. Consumer Corner: Canadian Pet Market Outlook, 2014. Alberta Agriculture and Forestry. http://www1.agric.gov.ab.ca/$department/ deptdocs.nsf/all/sis14914. Accessed: December 28, 2015.
2. Takashima GK, Day, MJ: Setting the One Health Agenda and the Human-companion Animal Bond. Int J Environ Res Public Health 2014; 11(11): 11110–11120.
3. Levine GN, Allen K, Braun LT, et al: Pet Ownership and Cardiovascular Risk: A Scientific Statement from the American Heart Association. Circulation 2013; 127(23):2353–2363.
4. Heady B, Grabka M, Kelley J, et al: Pet Ownership Is Good for Your Health and Saves Public Expenditure Too. Australian and German Longitudinal Evidence. Aust Soc Monit 2002; 5(4):93–99.
5. CHIRPP Injury Brief: Injuries Associated with Non-fatal Dog Bites. Public Health Agency of Canada. http://www.phac-aspc.gc.ca/injury-bles/chirpp/pdf/CHIRPP_INJURY_BRIEF_DOG_BITE_update.pdf. Accessed: December 28, 2015.
6. Ozanne-Smith J, Ashby K, Stathakis VZ: Dog Bite and Injury Prevention —Analysis, Critical Review, and Research Agenda. Inj Prev 2001; 7(4):321–326.
7. CHIRPP Database, Summary Data for 1996, All Ages. Injuries Associated with Dog Bites and Dog Attacks. CHIRPP Injury Report. http://www.phac-aspc.gc.ca/injury-bles/chirpp/injrep-rapbles/dogbit-eng.php. Accessed: January 1, 2016.
8. Weiss HB, Friedman DI, Coben JH: Incidence of Dog Bite Injuries Treated in Emergency Departments. JAMA 1998; 279(1):51–53.
9. Holmquist L, Elixhauser MA: Emergency Department Visits and Inpatient Stays Involving Dog Bites. Statistical Brief #101. 2010. In: Healthcare Cost and Utilization Project Statistical Briefs. Agency for Health Care Policy and Research, Rockville, MD.
10. Gilchrist J, Sacks JJ, White D, et al: Dog Bites: Still a Problem?. Inj Prev 2008; 14(5):296–301.
11. Part 1: Key Immunization Information 2013. Canadian Immunization Guide. Public Health Agency of Canada. http://www.phac-aspc.gc.ca/publicat/cig-gci/p01-12-eng.php#tab6. Accessed: December 27, 2015.
12. Moscati RM, Mayrose J, Reardon RF, et al: A Multicenter Comparison of Tap Water versus Sterile Saline for Wound Irrigation. Acad Emerg Med 2007; 14(5):404–409.
13. Baddour LM, Endom EE: Patient Information: Animal Bites (Beyond the Basics). UpToDate. http://www.uptodate.com/contents/animal-bites-beyond-the-basics. Accessed: December 29, 2015.
14. Paschos NK, Makris EA, Gantsos A, et al: Primary Closure versus Non-closure of Dog Bite Wounds. A Randomised Controlled Trial. Injury 2014; 45(1):237–240.
15. Talan DA, Citron DM, Abrahamian FM, et al: Bacteriologic Analysis of Infected Dog and Cat Bites. N Engl J Med 1999; 340(2):85–92.
16. Abrahamian FM, Goldstein EJC: Microbiology of Animal Bite Wound Infections. Clin Microbiol Rev 2011; 24(2):231–246.
17. De Serres G, Skowronski DM, Mimault P, et al: Bats in the Bedroom, Bats in the Belfry: Reanalysis of the Rationale for Rabies Postexposure Prophylaxis. Clin Infect Dis 2009; 48(11):1493–1499.
18. Part 4: Active Vaccines. Canadian Immunization Guide. Public Health Agency of Canada. http://www.phac-aspc.gc.ca/publicat/cig-gci/p04-rabi-rage-eng.php#ru. Accessed: December 30, 2015.
19. Rupprecht CE, Briggs D, Brown CM, et al: Use of a Reduced (4-dose) Vaccine Shedule for Postexposure Prophylaxis to Prevent Human Rabies: Recommendations from the Advisory Committee on Immunization Practices. MMWR Recomm Rep 2010; 59(RR-2):1–9.
Presented at the Dalhousie Continuing Professional Development Emergency Medicine Refresher on February 21, 2015.